Access to healthcare is, in theory, one of the most fundamental things a health system can offer. In practice, it’s one of the areas where the gap between intention and reality is widest. Improving patient access is a phrase that comes up constantly in NHS policy, in healthcare management discussions, and in the conversations I follow closely in my experience. But it’s one thing to identify access as a problem; it’s quite another to address it operationally.
If you’re working in healthcare operations or managing patient-facing services, and you’re exploring how specialist outsourced support can contribute to improving patient access, much of what follows will be directly relevant. For those curious about what quality call centres in South Africa can offer healthcare providers specifically, it’s worth understanding the broader access landscape first.
- The Scale of the Patient Access Problem Across UK Healthcare Services
- Where Dedicated Support Models Make the Most Difference for Patient Access
- Training and Cultural Fit: What Effective Healthcare Support Teams Actually Require
- Technology and Human Support Working Together for Improving Patient Access
- Equity and Inclusion: Making Improving Patient Access Work for Every Patient
- Keep Reading: Practical Insights on Healthcare Support at Customer Experience Online
The Scale of the Patient Access Problem Across UK Healthcare Services
The figures are stark and worth establishing clearly. According to the BMA’s NHS backlog data analysis, the NHS waiting list in England stood at approximately 7.29 million cases as of late 2025, comprising around 6.17 million individual patients. The median waiting time to start treatment was 13.4 weeks, compared to a pre-COVID median of 8.3 weeks. Around 139,000 patients have been waiting over a year for treatment, and patients waiting more than 12 hours for an emergency admission in January 2026 numbered 71,517 — approximately 25 times higher than in January 2020.
The access challenge isn’t confined to secondary care. According to the Care Quality Commission’s State of Care 2024/25 report, around 1 in 3 patients who tried to contact their GP by phone described the experience as difficult, with access consistently harder for those in the most deprived areas, autistic people, those with learning disabilities, and patients from certain ethnic minority backgrounds. These aren’t marginal disparities; they represent millions of people whose first point of contact with the health system is itself a barrier.
The administrative load compounds the clinical problem. Patients frequently struggle not just to access treatment but to navigate the system around it: booking appointments, understanding referral pathways, following up on test results, managing repeat prescriptions, or finding out where they are on a waiting list. Each of these touchpoints is an opportunity to either reduce or amplify the friction patients experience.
Where Dedicated Support Models Make the Most Difference for Patient Access
Dedicated patient support, whether delivered in-house or through a specialist outsourced partner, addresses a specific and underappreciated part of the access problem: the administrative and navigational layer that sits between the patient and the clinical care they need. When this layer functions well, patients reach the right service faster, with less confusion and fewer failed contacts. When it functions poorly, it creates unnecessary delays, frustrated patients, and additional pressure on clinical staff who end up fielding queries that shouldn’t have reached them.
The most effective dedicated support models in healthcare context handle appointment scheduling and rescheduling at scale, triage incoming contacts to direct patients appropriately, follow up on incomplete referral pathways, and provide clear, accurate information about waiting times and next steps. Done well, this doesn’t replace clinical judgment; it protects clinical time by ensuring that clinicians are dealing with clinical decisions, not administrative queries.
The NHS App improvements announced in 2025 offer a useful parallel. According to the UK government, app features have already saved almost 5.7 million hours of staff time and helped avoid 1.5 million missed appointments since July 2024, equivalent to an estimated saving of £622 million. The principle is the same whether the tool is digital or human: reducing friction in the access journey frees up the system to deliver more care.
Training and Cultural Fit: What Effective Healthcare Support Teams Actually Require
One of the most important things I come back to when advising on outsourced or dedicated support for healthcare organisations is that sector-specific training isn’t optional. A general customer service agent, however skilled, is not automatically equipped to handle healthcare contacts with the sensitivity, accuracy, and compliance awareness those interactions require.
Effective healthcare support agents need to understand the basics of NHS referral pathways, the language of clinical administration, data protection obligations specific to health information, and the emotional register appropriate for patients who may be anxious, unwell, or frustrated. An agent who handles a cancer referral query with the same tone as a billing enquiry is not delivering healthcare-appropriate support, regardless of how efficiently the contact is resolved.
Cultural fit matters too, particularly in the context of offshore or nearshore delivery. The best offshore support teams I’ve seen operating in healthcare have invested heavily in UK-specific cultural and procedural training: understanding how the NHS works, what patients expect from it, and how to communicate in a way that feels empathetic and appropriate to someone navigating a health concern. That investment is what separates effective healthcare support delivery from generic contact centre work dressed up in clinical language.
Technology and Human Support Working Together for Improving Patient Access
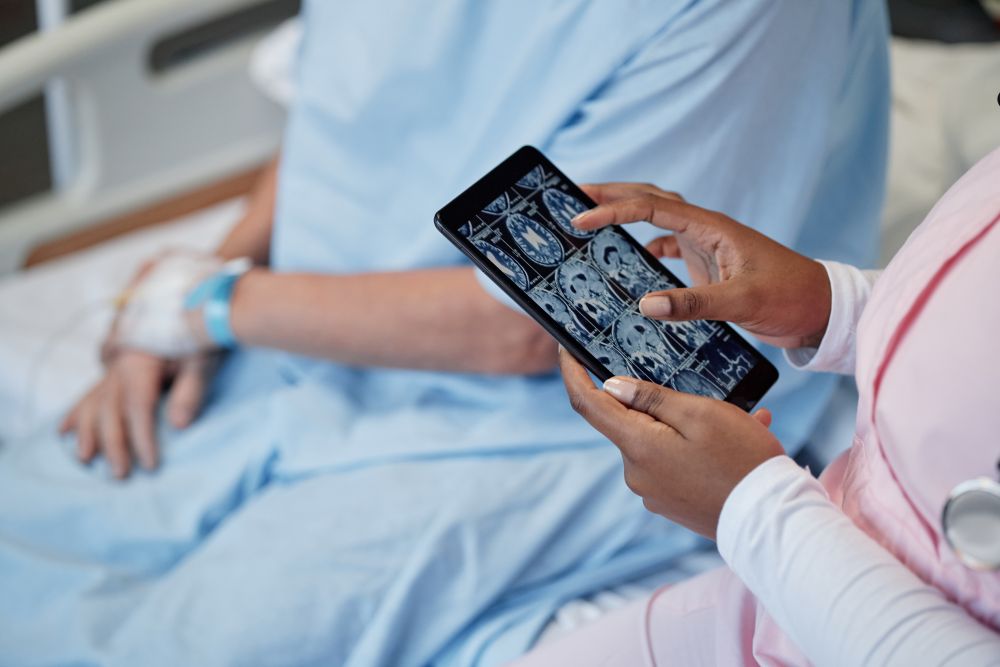
The most sophisticated approaches to improving patient access combine human support with intelligent technology rather than treating them as alternatives. Automated systems handle routine, high-volume contacts: appointment confirmations, prescription renewal reminders, waiting time updates. Trained agents handle the contacts that require empathy, judgment, and nuanced communication, which in a healthcare context is a significant proportion of the total.
Real-time dashboards that give managers visibility of contact volumes, resolution rates, and escalation patterns are particularly valuable in healthcare settings where demand can shift rapidly. Knowing in real time that a particular service or pathway is generating disproportionate contact volume often signals an upstream problem that can be addressed before it becomes a patient safety concern. That kind of operational intelligence doesn’t emerge from a disconnected support model; it requires integrated reporting and a team that understands what it’s looking for.
I’ve written more on the importance of managing service delivery across multiple markets and the same logic applies directly within complex healthcare environments, where different services, specialties, and geographies all generate different patterns of patient contact that need to be managed distinctly rather than homogenised.
Equity and Inclusion: Making Improving Patient Access Work for Every Patient
Any serious approach to improving patient access has to grapple with the equity dimension. The Nuffield Trust and Health Foundation’s QualityWatch analysis found that Black children and young adults between the ages of 0 and 19 wait an average of 21 minutes longer in A&E than white patients the same age. Patients from the most deprived areas are disproportionately likely to be waiting for planned care. These disparities are not simply clinical; they reflect access barriers that well-designed support systems can help address.
Multilingual support capability, extended hours coverage, and accessible contact channels all make a tangible difference to the patients most likely to face barriers. A healthcare support model that operates only in English, only during standard working hours, and only via phone is structurally less accessible than one that offers multiple languages, extended availability, and digital channel options. That isn’t a nice-to-have; it’s a core component of what equitable patient access actually means in practice.
The offshore model, when structured and trained correctly, can contribute meaningfully here. Multilingual capability at scale is easier to achieve through a large offshore operation than through a small in-house team, and extended hours coverage becomes economically viable when it isn’t carrying the full cost overhead of domestic staffing rates.
Keep Reading: Practical Insights on Healthcare Support at Customer Experience Online
If this piece has got you thinking about how your own patient support model is structured and where it could do more, there’s a lot more to explore at Customer Experience Online. We publish regular, evidence-based content on the full range of customer and patient experience challenges facing healthcare and other regulated sectors. From building offshore support models that meet compliance requirements to measuring service performance in ways that reflect real patient outcomes, our content is designed to give you something genuinely useful. Browse our latest pieces and bookmark the site so you don’t miss what’s coming next. Whether you’re planning a new support model or reviewing an existing one, you’ll find practical guidance rooted in real operational experience.
Frequently Asked Questions (FAQs)
It refers to a support model specifically trained and resourced to handle patient-facing administrative and navigational tasks: appointment scheduling, referral follow-ups, waiting time queries, and signposting to the right services. Done well, it reduces friction in the patient journey and frees up clinical staff for clinical work.
By providing scalable, cost-effective capacity for high-volume administrative contacts that would otherwise absorb clinical or in-house staff time. Specialist outsourced partners with healthcare sector training can handle these contacts consistently, at extended hours and across multiple channels, without the overhead of equivalent domestic headcount.
Sector-specific training covering NHS referral pathways, clinical administration language, data protection obligations under UK GDPR and the Data Protection Act, and the emotional register appropriate for patients in distress. Generic customer service skills are a foundation, not a substitute for this specialised preparation.
Yes, provided the offshore partner has demonstrable experience in regulated healthcare environments and robust compliance frameworks in place. Data handling, access controls, and staff training must all meet the relevant UK and sector-specific standards. Partner selection should include thorough due diligence on compliance infrastructure, not just cost and capacity.
Multilingual capability, extended hours, and accessible digital channels all reduce the structural barriers that disproportionately affect patients from deprived areas, minority ethnic communities, and those with disabilities. A well-designed support model actively addresses these disparities rather than replicating the access gaps already present in the system.




